“We've crushed the flu this year. The rate of influenza this year is over 100 times lower than it’s ever been. Why did this happen? It’s obvious: all of the precautions we’re taking to reduce the spread of Covid-19 have worked wonders to prevent the flu as well. In fact, they’ve worked far better for influenza than for the Covid-19 virus.”(1)
So says a gentleman called Steven Salzberg in Forbes magazine. It's a low resolution explanation, but touching nonetheless. However, could it be possible that precautions that don't work for one highly infectious respiratory disease do work for another instead? And, in the light of our new found devotion to vaccines, what effect has the annual flu vaccine had on proceedings, both last season and this?
Well, the US flu season 2020-21 is undoubtedly at a record low. It almost goes without saying, but the following numbers need to be treated with a good deal of skepticism. The Centre for Disease Control are the ones providing them and their not particularly well hidden agenda is to persuade the population to get a flu jab.
In the previous ten seasons, the number of hospitalizations and deaths have trended between estimated totals of 808,000 and 61,000 (2017-18) respectively and 140,000 and 12,000 (2011-12). It can therefore be seen that the difference between a severe season and a mild season is considerable.
Between 10/1/20 and 16/1/21, the CDC recorded only 136 hospitalizations and 292 deaths. That trend has continued, and the current weekly update (end March 2021), shows the hospitalization rate hovering at 0.7 persons per 100,000. This is just a fifth of the rate for 2011-12, an exceptionally mild season.
And it's not just the US; during the Southern Hemisphere's winter (our summer), Australia kicked off the season with 14 recorded cases in April (as against 369 the year before) and by June, peak season, that number had declined to zero, where it remained from July to October. Chile recorded 12 cases between April and October, as opposed to 7,000+ the year prior. South Africa had similar results and, globally, it was estimated that by October 2020, recorded cases of flu were down 98% compared to 2019.(2)
Why? In one scenario, scientists speculate that there is possible pathogenic competition between the two viruses and that Covid is winning the battle, on the basis that co-infection is strikingly rare. There is some foundation to this theory as a Chinese study found that, with both SARS and MERS (two previous viral outbreaks) natural infection with another virus, such as the flu, provides some protection against a coronavirus. Whether that study can be replicated and whether the process works both ways around is not known and, in any event, estimated Covid infection rates at the beginning of the flu season were about 15-20%, not high enough to prevent flu by interference.
Another possibility, that you or I might entertain, is that flu cases are being counted as Covid 'cases', given the similarity in the symptoms presented by each virus. The scientific community has dismissed this possibility, stating that the two viruses look completely different under a microscope. However, not all PCR tests are sent to a laboratory; the antigen tests, those used at airports for example, are not. And not all patients whose deaths have been recorded as being due to Covid have even been tested.
Their best guess is that hand-washing, social distancing, lock-downs etc. have been effective against the flu...but, apparently, not against Covid. As a scientific explanation (which, you would think, is what scientists are in the business of providing), this seems less than compelling.
But, here is where the infamous R number makes an appearance. This number (well, two numbers combined– Ro and Re) reflects the infectivity of a disease. Apparently, Covid is more infectious that the flu. Covid has an R number of 2.63 and flu has an R number of 1.3, meaning that (on average) a person infected with Covid gives the virus to twice as many people as a person who has the flu and that's why Covid has still proliferated whereas the flu has died a death. Except the estimates of the Covid R number range from 0.4 to 4.6 and the flu Ro varies every year, so no clear comparison can, in fact, be made.(3)
“The R number is imprecise, not current, an average that hides local variation – a bad tool on which to base policy.”(4)
As an aside, a friend's wife got Covid – not just a positive PCR test, symptoms as well such as a loss of smell and taste. None of her husband, daughter or granddaughter developed any symptoms or tested positive, despite making no effort to isolate. This is not to infer that Covid isn't infectious, merely that there are clearly other factors in play that have a bearing on its transmissibility.
The influenza disappearing act has not been covered in the press to any great degree. You might have thought it would be, as it's unprecedented, but no. Nobody seems to want to acknowledge the elephant in the room... and, as is often the case, the questions that are not being asked are as important as the ones that are.
Both the CDC and the UK National Health Service stopped counting flu cases in October 2020, which is also a first and difficult to understand as it would surely be important to know what the relationship between the two viruses is. Additionally, flu testing was down but not, one suspects, by 98%. So is the flu out there, or not? Could it not be mistaken for Covid in people that aren't tested, but are nonetheless diagnosed? As the mechanisms for testing and estimating flu rates rest with the authorities, who seem to have abrogated their responsibility, these questions cannot be definitively answered...which may be the point.
There is a further element to the flu/Covid dynamic and that is the probable impact of the flu vaccine on the severity of Covid symptoms in elderly patients. In the US, over 65s get a high dose flu vaccine called Fluzone High-Dose Quadrivalent. As the name suggests, it contains four times the antigen, to stimulate a stronger immune response and is allegedly 24% more effective. This process is repeated in many western countries. And every year, there are a spate of deaths in care facilities, right after vaccinations.(5)
Indeed, there is a significant worldwide positive association between Covid 19 deaths and flu vaccines in people over 65.(6) Another study, published in October 2019 (in plenty of time to effect decision making for the 2020-21 flu season, if not the one before) demonstrated that influenza vaccinations interfered significantly with the chances of subsequently contracting a coronavirus infection (36% more likely) or human metapneumovirus (51% more likely).(7) Incidentally, this latter disease has similar symptoms to Covid 19.
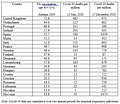
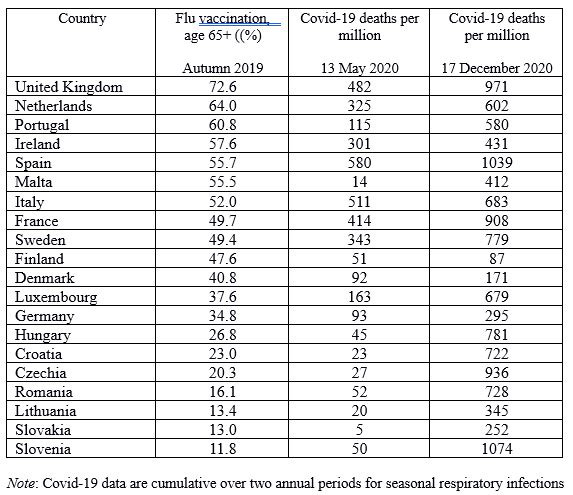
Table 1 below (8) shows a direct correlation between countries with extensive flu vaccination programmes for the elderly and Covid deaths, for the 2019-20 flu season. Once more, caution must be exercised as not all countries recorded deaths in the same way, but the trend is, nonetheless, striking. It is also noticeable that Eastern European countries seem to have have had far more problems in the first half of the 2020-21 season than the year previously. Whilst the causation is not definitive at present (and may never be), it is noteworthy that the WHO was vigorously promoting flu vaccines this season and, further, that the take-up was sufficiently inflated as to cause supplies to run low.
And it's not just the elderly who are at increased risk from flu vaccinations. An extensive study of flu vaccinations in children found that those that were vaccinated (as against the control group who remained unvaccinated) had a five-fold increase in the risk of contracting other acute respiratory viruses, including coronaviruses. The conclusion was that, despite being
“protected against influenza....recipients may lack temporary, non specific immunity that protected against other respiratory viruses.”(9)
To a layperson, this statement makes sense. Wouldn't you expect to be a little vulnerable to other viruses if your body was busy creating antibodies to the flu? Or, alternatively, as both the flu and a coronavirus are respiratory viruses, might there a possibility of the immune system becoming overwhelmed if both viruses presented at the same time?
We are left with more questions than answers. It seems highly probable that flu vaccinations result in increased risk of a coronavirus infection or pneumonia in both young and old, with the elderly being more vulnerable to fatal outcomes. Could it be that rather than succumbing to a flu infection, this group died of Covid instead and that, last year and this, their numbers have been swelled by either two different vaccinations (this year) or a flu jab and a Covid infection?
Or is it the case that the flu estimates of previous years were grossly overstated in an attempt to 'persuade' the over 65s to get a jab and the numbers for this season are, in fact, correct?
Alternatively, is it probable that not all the deaths attributed to Covid were, in fact, Covid? Given that some were diagnosed without the evidence of a test, unreliable though the tests were and are, and the fact that symptoms for Covid, flu and pneumonia are very similar, it would seem highly likely.
If the responsibility for recording the numbers is in the hands of organisations that have forfeited a degree of trust, due to inaccurate projections and what can only be described as fear mongering, how are we going to know?
The most important question, which hovers over every aspect of this pandemic, is about how so many actions seem to be ill considered, ignorant of the evidence and either not fully explained or misleadingly presented. Why is that?
Citations
Steven Salzberg, Forbes Magazine, March 8th 2021
Mail Online, 20/10/2020.
BMJ 2020; 369;m1891
Nature Magazine A guide to R – the pandemic's misunderstood metric – David Adam 3/7/20
Wehenkel C. 2020. Positive Association between Covid 19 deaths and influenza vaccinations in elderly people worldwide. PeerJ8:e10112 DOI 10.7717/peerj.10112)
Wolff, Influenza Vaccination & Respiratory Virus Interference Among Department Of Defence Personnel During The 2017/2018 Influenza Season
Cowling, et al Increased Risk of Non Influenza Respiratory Virus Infections Associated With Receipt Of Inactivated Influenza Vaccine OUP. DOI:10.93/cid/cis307